Sarcoids in horses
Sarcoids are by far the most common skin cancer in horses with some reporting them to account for 90% (results spanning from 36-90%) of all skin neoplasms in horses. They affect all equids and all breeds with no age or sex predisposition. There are numerous published or anecdotally reported treatments which reflects the variable efficacy of available treatments with none being universally successful. Sarcoids can be benign and remain so or can become extensive and debilitating. Therefore the key message is that early accurate treatment increases the chances of resolution dramatically.
What causes sarcoids in horses?
The pathogensis of sarcoids in horses is a complex and involves many factors.
- Bovine papillomavirus (BPV) types 1 and 2 have been widely implicated as a causative agent of sarcoids. However when studies were carried out to induce sarcoid development with the virus the sarcoids regressed spontaneously. Therefore there must be added factors that result in the development and progression of sarcoids in some horses. In a study in 2001 BPV was found in 98% of sarcoids.
- A genetic predisposition – in a study done on 222 horses there were 3 chromosomes highlighted as sarcoid signalling genes. Further studies will be needed to establish if these genes are responsible for the development of the disease.
- Inoculation the virus into the skin – This can be a trauma, inflammation of the skin, flies, direct contact etc.). Sarcoids are associated with wounds and areas of irritated/inflamed skin. Flies have also been implicated with one study on 500 flies from an area with sarcoid affected horses indicated 98% of those tested were positive for BPV.
So although there is no exact cause there are well defined risk factors and the disease undoubtedly has a multifactorial aetiology.
There are 6 types of sarcoids:
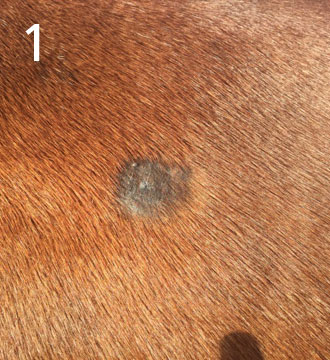 Occult (pic1) – Present like circular, flat, grey and hairless areas. Predilection sites are the neck, the mouth, the eyes and other hairless areas e.g. the armpit. Although often slow growing, they can often progress to verrucose sarcoids or if traumatised can become fibroblastic (explained below)
Occult (pic1) – Present like circular, flat, grey and hairless areas. Predilection sites are the neck, the mouth, the eyes and other hairless areas e.g. the armpit. Although often slow growing, they can often progress to verrucose sarcoids or if traumatised can become fibroblastic (explained below)
 Verrucous (pic2) – Wart-like sarcoid that can be flat or have a narrow neck, so some may look like real warts whilst others look like scabby skin. Predilection sites include the face/body groin and sheath. They can be small and well defined but some extend over large ill-defined areas. Similarly if traumatised they can develop into the fibroblastic form.
Verrucous (pic2) – Wart-like sarcoid that can be flat or have a narrow neck, so some may look like real warts whilst others look like scabby skin. Predilection sites include the face/body groin and sheath. They can be small and well defined but some extend over large ill-defined areas. Similarly if traumatised they can develop into the fibroblastic form.
Nodular – Firm well defined round nodules under the skin. Predilection sites include the groin sheath and eye. There are 2 different types, /type A is freely moveable under the skin, whilst type B are more involved in the deeper layers of tissue. Type A is easier to treat. The number of nodules varies widely. The skin may become thin and this leads to ulceration and bleeding, this may also occur after trauma.
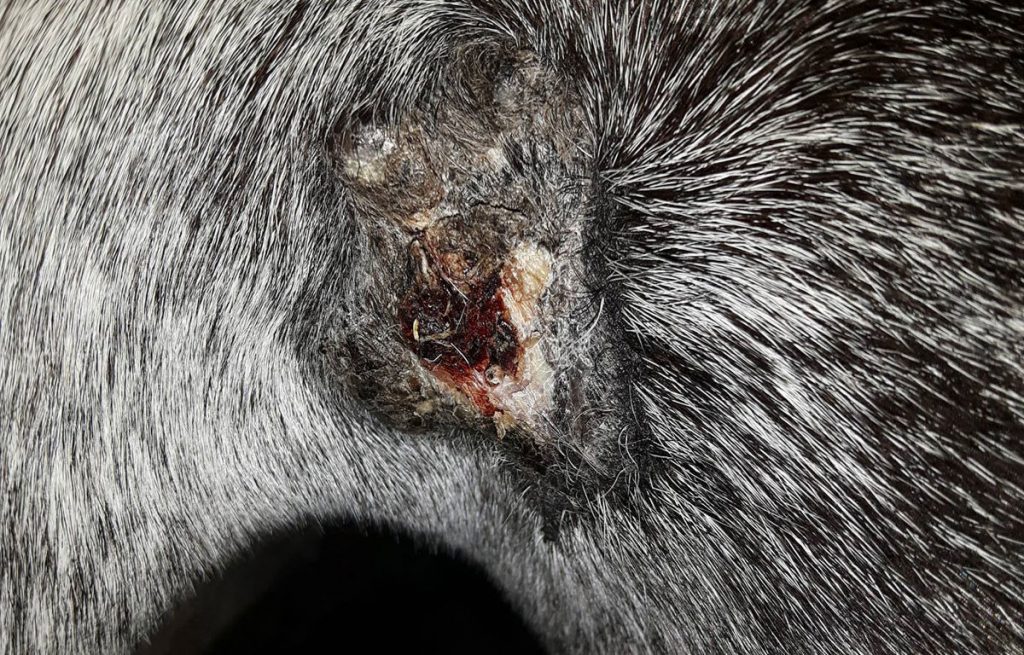
 Fibroblastic (pic3) – Fleshy mass with a bleeding and ulcerated surface which results in an aggressive and unsightly appearance. Type 1 has a narrow base, whilst type 2 has a broad invasive base. Common sites include the axillae, groin and around they eye. Often result from damage to other more benign sarcoids. They are also common at wound sites (even surgical ones) and should be considered with non-healing wounds. Local invasion can occur and is worsened if the sarcoid is traumatised which can occur particularly with non-healing wounds as it looks so similar to proud flesh.
Fibroblastic (pic3) – Fleshy mass with a bleeding and ulcerated surface which results in an aggressive and unsightly appearance. Type 1 has a narrow base, whilst type 2 has a broad invasive base. Common sites include the axillae, groin and around they eye. Often result from damage to other more benign sarcoids. They are also common at wound sites (even surgical ones) and should be considered with non-healing wounds. Local invasion can occur and is worsened if the sarcoid is traumatised which can occur particularly with non-healing wounds as it looks so similar to proud flesh.
Mixed – Usually occurs in sarcoids that are in a progressive state between types of sarcoids e.g. occult to verrucous usually as a result of irritation.
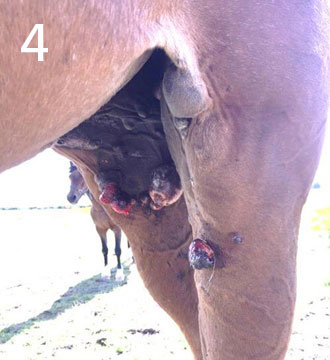
Malignant (pic4) – This is a rare aggressive locally invasive tumour. The sarcoid can extend widely along the skin and even invade the lymphatic vessels. Malignant tumours are dangerous and notoriously hard to treat. A history of repeated trauma particularly surgical excision attempts is common.
Diagnosing sarcoids in horses
Sarcoids are most commonly diagnosed appearance, location and clinical history. Definite diagnosis of a sarcoid is achieved with a biopsy. However, as indicated several times above trauma to a sarcoid can make induce a more aggressive form of the disease. A swab of the lesion or a superficial scraping can be sent for testing for the presence of BPV, this test can be expensive and is not always available. Therefore early consultation of your vet on any lesion that looks suspicious is essential.
Treatment of sarcoids
NOTE: Failure to resolve the lesion results in a drop in prognosis of 40% with each attempt.
The sarcoid will be more aggressive and more resilient to treatment. Therefore the first treatment of the sarcoid must be most likely to work. I can’t emphasis this enough and would love you to keep it in mind when reading the possible treatments available.
There are so many treatments available for sarcoids (which is always a bit disconcerting), that I have chosen a selection that I feel are or could be used here in Ireland.
- Surgical excision – Surgical excision without adjunctive therapy has the highest (50-64%) recurrence rate. Malignant cells can often be projecting into surrounding tissue, growth factors of healing can stimulate latent viral infections associated with sarcoids and slow healing wounds or partially healing wounds are perfect sites for sacroid growth. Specfic types of nodular sarcoid can be excised with a good success rate and it is also beneficial when used to enable other treatments to be more effective.
- Laser surgery – lesion selection is very important, similar to surgical excision. However it does have the advantage of faster healing wounds and the heat kills surrounding cells which decreases recurrence rate. In a study of 99 horses there was 83% success rate.
- Cryotherapy – The depth and duration of freeze is very important and multiple treatments are often necessary. Success is very vet dependent with reports varying widely (literally 1-100%). In one particular study on peri-ocular occult sarcoids 91% had aggressive regrowth within 12 weeks of treatment.
- Cytotoxic/Anti-mitotic compounds (Liverpool cream) – These creams inhibit cell division and growth. It has been shown to prevent regression in 35-80% of lesions in 2 different studies. They can be associated with pain, scarring and swelling. Thus it is not advised for peri-ocular or coronary band lesions. Also the substance is highly toxic and thus is a veterinary only product.
- Topical Immiquimod – This cream modifies the immune response and has potent antiviral and antitumour activity. In a study of 19 tumours there was complete resolution of 60% of cases. The cream can be applied by the owner but treatment can last for up to 32 weeks.
- Intralesion infiltration of chemotherapy drugs – Cisplatin and 5-Fluorouracil are the drugs that are used. Cisplatin in a study of 409 sarcoids 96.3% went into complete remission. However, it is intensely carcinogenic to humans and thus if best avoided if possible. Fluorouracil is been used more frequently particularly for peri-ocular lesions. In one study it resulted in 61.5% of cases.
- Electrochemotherapy – is a combination of chemotherapy in the form of cisplatin and electrical field pulses that allow penetration of the drug. The treatment is every 2 weeks and varies in longevity. In a study done of 194 sarcoids on 48 equids there was a 99.5% success of sarcoid regression. However general anaesthesia is necessary which increases costs and risks.
- Xxterra – an ointment containing zinc chloride and extract of bloodroot. In open pilot study on 16 sarcoids there was a 62% success rate with only one of those sarcoids relapsing after 35months. However the treatment can be as long as 6 months and damage to the deeper tissues has been anecdotally reported.
As you can see from the statistics and long list of treatments there is no treatment protocol that is universally effective. Even during my research on this topic there was a constant inconsistency with therapeutic efficacy. Treatment selection is sarcoid, horse and client dependent. Therefore veterinary advice before the use of any remedies is strongly recommended.
Although sarcoids can be extremely persistent and can cause ongoing difficulties for both horse and rider, treatment can be extremely effective, as shown by a recent case report on sarcoids, of a horse treated at Greenmount Equine Hospital, which you can see here.
Please note that our veterinary articles are written to give you insights and understanding of common equine veterinary problems and are not intended to take the place of a veterinary examination by your own vet. If in doubt, always call your own vet should your horse require attention.
Nikki Walshe MVB is a resident vet at Greenmount Equine Hospital, Limerick
Share this article with fellow horse lovers by using the share buttons below.

Cause Of Swollen Sheath In Horses | Erectile Dysfunction Cure Exercise
September 30, 2016 at 1:48 pm[…] Sarcoids in horses – Predilection sites include the face/body groin and sheath … sarcoid, horse and client dependent. Therefore veterinary advice before the use of any remedies is strongly recommended. Although sarcoids can be extremely persistent and can … […]